Breathing Techniques for Digestion (2026 Guide): GERD Relief, Vagus Nerve Support, and a Simple 3-Minute Humming Add-On
Digestion isn’t only about what you eat — it’s also about how your nervous system is behaving while you eat. If you’re stressed, rushed, or breathing high in the chest, your gut can feel slow, tight, or reactive. This guide pulls together practical, research-supported breathing techniques that may help support calmer digestion, including gentle options for reflux (GERD), bloating, and that “wired but tired” feeling that makes meals sit heavy.
If you buy through our links, we may earn a small commission at no extra cost to you. We only recommend resources we genuinely believe can support a healthier, calmer life.
Quick Answer
If you want one simple breathing strategy for digestion, start with diaphragmatic (belly) breathing and a longer exhale. Evidence suggests diaphragmatic breathing training can reduce belching and reflux symptoms in some people with PPI-refractory GERD (especially when supragastric belching is involved). Add a short humming practice after your session — humming has been shown to increase nasal nitric oxide about 15-fold during the hum compared with quiet exhalation, and many people experience it as a calming “reset.”
At a Glance
- Best starting point: 3–5 minutes of diaphragmatic breathing before meals
- If you deal with reflux/GERD: breathe low and slow; avoid tight belly bracing; consider a post-meal gentle walk
- If you swallow air (burping/bloating): slow the pace and reduce mouth-breathing (aerophagia is common when we rush or breathe fast)
- Fastest add-on: 3 minutes of humming (“mmm” on the exhale)
- Food support that pairs well: simple meals, enough fiber, fermented foods if tolerated; be careful with peppermint if reflux is your main issue.
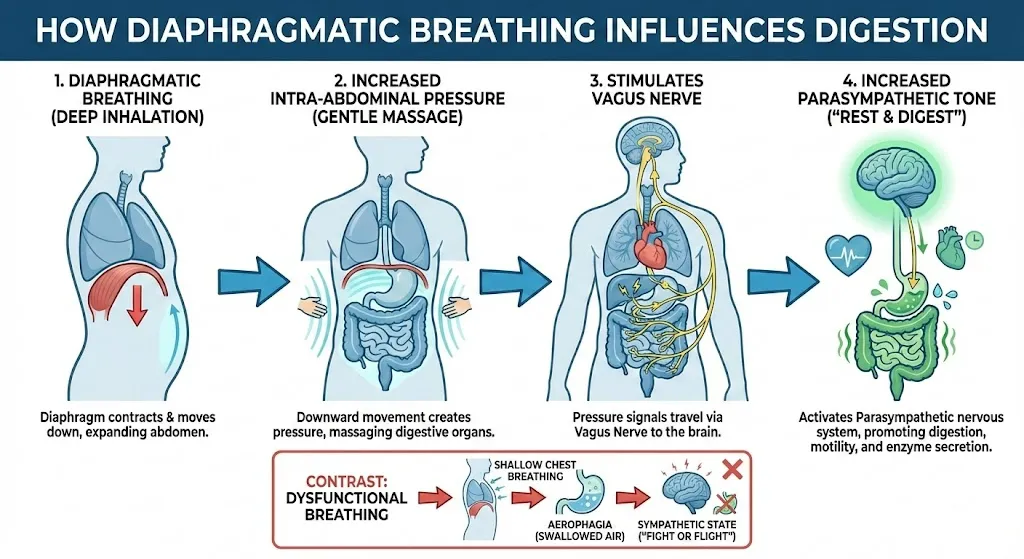
Why breathing affects digestion more than most people realize
Your digestive system is heavily influenced by the autonomic nervous system — the same system that shifts you between “go mode” (sympathetic) and “rest-and-digest” (parasympathetic). The vagus nerve is a major communication pathway between brain, heart, and gut, and it plays a key role in parasympathetic regulation.
When you’re rushed or anxious, it’s common to:
- breathe faster or higher in the chest
- swallow more air
- tense the abdominal wall
- eat quickly (which adds even more swallowed air)
This doesn’t mean breathing is a magic fix. But it does mean that changing your breathing can be a practical, low-risk way to support better conditions for digestion.
GERD basics, in a calm and practical way
GERD (gastroesophageal reflux disease) is common and usually managed with a combination of lifestyle strategies and (when needed) medications like PPIs. The American College of Gastroenterology guideline includes practical recommendations for evaluation and treatment, and also highlights when “alarm symptoms” require medical review (like trouble swallowing, bleeding, or unexplained weight loss).
A key idea for reflux: anything that increases pressure upward or relaxes the lower esophageal sphincter (LES) can make symptoms worse for some people. That’s one reason peppermint can be tricky: it may relax the LES and worsen reflux in susceptible people.
So when we talk about breathing for GERD, the goal is not “force more air.” The goal is often:
- less strain (especially in the belly and throat)
- less air swallowing
- more relaxed, lower breathing
Diaphragmatic breathing is one of the most effective tools in our Breathing Techniques library
Breathing Techniques that support digestion (without hype)
Below are the core practices that tend to help the widest range of people. Start with the first two before you experiment with anything more intense.
1) Diaphragmatic (belly) breathing
This is the foundation. In simple terms: your belly gently expands on the inhale, and softens on the exhale. You’re reducing upper-chest effort and letting the diaphragm do more of the work.
Why this matters for reflux and belching: in a prospective study, a standardized diaphragmatic breathing training protocol reduced belching and reflux symptoms in a group of patients with PPI-refractory GERD (especially those with excessive supragastric belching).
How to do it (2 minutes):
- Sit upright with a relaxed jaw and shoulders.
- One hand on the belly, one on the chest.
- Inhale through the nose: try to move the belly hand more than the chest hand.
- Exhale slowly through the nose (or softly through pursed lips if your nose feels blocked).
- Keep it easy. No “big performance breath.”
2) Longer exhale breathing (the quickest calming lever)
A longer exhale is one of the simplest ways to shift your body toward “safe enough to digest.”
Try this:
- Inhale 3–4 seconds
- Exhale 6–8 seconds
- Repeat 6–10 times
If you tend toward reflux, avoid clenching your abs on the exhale. Think: “soft belly.”
Calming the breath helps calm the mind. Learn how breathing builds mental resilience
3) Pursed-lip breathing (useful if you feel tight or air-hungry)
This can be helpful when your breathing feels shallow, anxious, or “stuck.”
How:
- Inhale through the nose for 2 counts
- Exhale through gently pursed lips for 4 counts
It slows you down and often reduces the urge to gulp air.
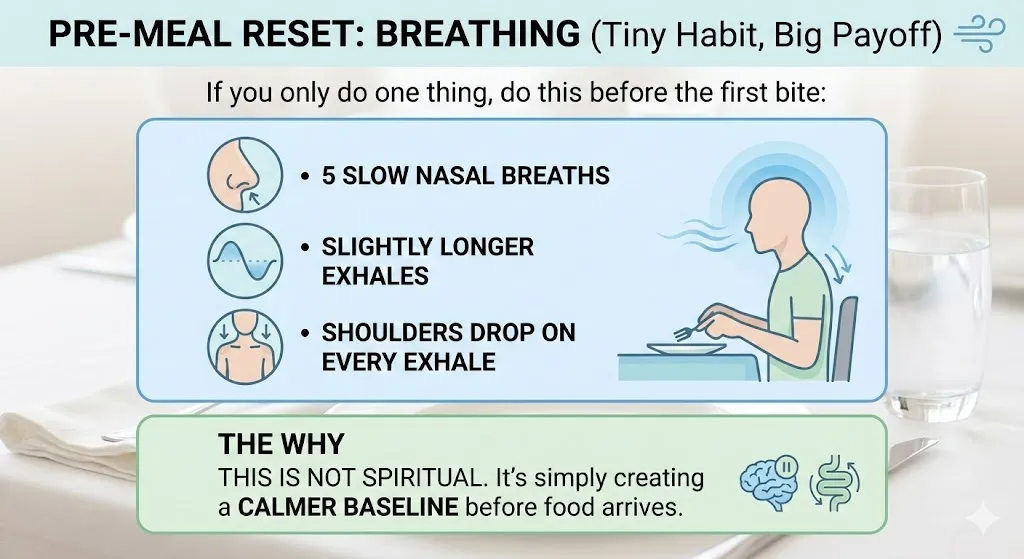
4) “Pre-meal reset” breathing (tiny habit, big payoff)
If you only do one thing, do this before the first bite:
- 5 slow nasal breaths
- slightly longer exhales
- shoulders drop on every exhale
This is not spiritual. It’s simply creating a calmer baseline before food arrives.
Breathing works best alongside proper nourishment. Explore Nutrition & Support strategies
Aerophagia: the hidden reason some people feel bloated from “breathing exercises”
If you’re burping a lot or feeling gassy after breathwork, you might be swallowing air. Aerophagia is the medical term for excessive air swallowing, and it can contribute to belching, bloating, and discomfort.
Common causes include fast breathing, mouth-breathing, rushed eating, anxiety, and even certain breathing patterns that encourage “gulping.”
If you suspect aerophagia:
- slow the pace
- keep the inhale softer
- try nasal breathing more often
- stop the session if you feel pressure building in the upper belly
Certain foods naturally reduce bloating. See our guide to Functional Foods for digestion
My personal 20-minute morning routine (free, anywhere)
In my own routine, I do Wim Hof–style breathing in the morning, and right after I add about 5 minutes of gentle humming. All together it takes me around 20 minutes, and I love it because it doesn’t require equipment, perfect weather, or a “wellness lifestyle.”
If you’re short on time, start smaller:
- 5–7 minutes total (short breath session + 1–2 minutes humming)
Safety note: Wim Hof Method breathing can rarely lead to fainting, and the official guidance warns this is especially dangerous around water (risk of drowning). Practice seated or lying down, never in/near water, and never while driving.
If you’re pregnant, have uncontrolled blood pressure, seizures, serious heart rhythm issues, or you’re unsure — ask a qualified clinician before doing intense breathwork or breath holds.
Anita’s 3-Minute Humming Add-On (right after breathwork)
This is the simple “landing” practice I use. It’s gentle, surprisingly calming, and easy to do anywhere.
A classic study found that humming increased nasal nitric oxide about 15-fold during the hum compared with quiet exhalation. PubMed+1 Nitric oxide is a signaling molecule involved in multiple body systems — but you don’t need to chase numbers here. The practical value is that humming naturally slows the exhale and adds a soothing vibration many people find regulating.
Step-by-step (3 minutes):
- Set posture (15 seconds): sit tall, relax jaw, lips gently closed.
- Nasal inhale (3–4 seconds): soft inhale, no “big breath.”
- Humming exhale (6–10 seconds): quiet “mmm” like a soft bumblebee.
- Repeat 10–12 cycles: if it feels strained, shorten the exhale.
- Finish with 3 silent breaths: notice throat, chest, belly.
1-minute emergency version:
6 slow breaths total: inhale 3 seconds → hum 6 seconds.
Family-friendly option: children and older adults can do humming + slow nasal breathing only (skip intense breath holds). Keep it playful and brief.
Herbs can gently support digestion and relaxation. Discover our Herbal Powerhouses
Optional but fascinating: why “Om” ends in a long “Mmmm”
“Om/Aum” has deep spiritual roots, but the “Mmmm” part is also mechanically interesting: it creates oscillating airflow and vibration that can increase nasal nitric oxide during the hum.
There’s also early neuroimaging research: a pilot fMRI study reported deactivation in several limbic brain areas (including the amygdala) during “Om” chanting compared with rest and compared with a control sound. This doesn’t prove a medical effect — but it supports why many people experience chanting as a calming “switch.”
If “Om” feels too spiritual for you, keep it simple: just hum “mmm.”
Food support that pairs well with digestion-focused breathing
Breathing helps create the state for digestion. Food choices help create the materials for digestion. You don’t need perfection — you need patterns.
If reflux is your main issue
- Consider smaller evening meals and give yourself time before lying down (many people notice a difference)
- Be cautious with peppermint if it worsens your symptoms, since it may relax the LES in some people.
- If symptoms are frequent or severe, use clinical guidance rather than guessing (GERD guidelines exist for a reason).
If bloating is your main issue
- Slow meals down (air swallowing matters more than most people think).
- Try a “breathing pause” halfway through your meal (3 slow breaths)
- Pay attention to which fibers and fermented foods you tolerate best
Probiotics and gut health (without the hype)
“Probiotics for gut health” can mean supplements — but it can also mean starting with foods:
- live yogurt/kefir (dairy or non-dairy), sauerkraut, kimchi, miso (as tolerated)
- prebiotic fibers from plants (oats, legumes, onions/garlic if tolerated, chia/flax, cooked-and-cooled potatoes/rice)
If you try a probiotic supplement, introduce one product at a time and track your response for 2–3 weeks. If you feel worse, stop and reassess.
Gentle teas and herbs
A warm tea can pair beautifully with slow breathing because it reinforces “safe, soft, warm.”
- ginger tea (often soothing for nausea)
- chamomile (many people find it calming)
- fennel (traditional for gas/bloating)
If reflux is active, test slowly and avoid anything that reliably triggers you.
When breathing won’t be enough (and you should get checked)
Breathing can be supportive, but it’s not a substitute for medical care. Please seek medical evaluation if you have:
- trouble swallowing, food sticking, vomiting blood, black stools
- unexplained weight loss
- persistent chest pain
- reflux symptoms that are frequent, severe, or worsening despite lifestyle changes
GERD guidelines emphasize proper evaluation, especially when alarm symptoms are present.
Breathing is foundational movement. Explore Exercise & Rehab resources
FAQs
Can breathing exercises stop acid reflux?
Breathing can’t “cure” GERD, but diaphragmatic breathing training has shown benefit for some people — especially where belching and reflux symptoms are linked to breathing patterns and supragastric belching.
What are the best breathing exercises for belching?
Start with slower diaphragmatic breathing and reduce mouth-breathing. Excess air swallowing (aerophagia) is a common contributor to belching.
How do I stimulate the vagus nerve for digestion?
The vagus nerve is deeply involved in parasympathetic (“rest-and-digest”) function. Practices that slow and lengthen the exhale — including gentle humming — are often experienced as calming and may support a digestion-friendly state. (Avoid treating it like a medical device; keep it gentle and consistent.)
Why do I feel more bloated after breathwork?
You may be swallowing air (aerophagia), especially with faster mouth-breathing. Slow down, keep the inhale softer, and stop if pressure builds.
Is peppermint tea good for digestion?
Peppermint can help some digestive discomforts, but it may worsen reflux in some people by relaxing the lower esophageal sphincter. If GERD is your issue, test cautiously or choose a different tea.
How long should I practice before I notice a difference?
Many people feel calmer after one session. For digestion-related benefits, think in weeks: small daily practice before meals is often more meaningful than one long session.
Conclusion
Breathing techniques won’t replace medical care or erase every digestive issue — but they can be a powerful, free way to support the conditions your gut tends to prefer: calmer nervous system tone, less air swallowing, and more relaxed abdominal pressure. Start with diaphragmatic breathing, add a longer exhale, and if you want a simple “landing,” use the 3-minute humming add-on. Over time, small consistent practice usually beats intensity.
About The Author
Anita Lauritsen
Anita Lauritsen is the founder of BreathFullLiving.com, a space devoted to exploring the connection between air, breath, and well-being. After surviving early-stage lung cancer and undergoing a lobectomy, Anita was inspired to share her journey and advocate for greater awareness of lung health. Through her writing, she offers compassion, insight, and practical guidance for anyone seeking to breathe more fully—both in body and in life.








